Bilateral pars defect1/8/2024  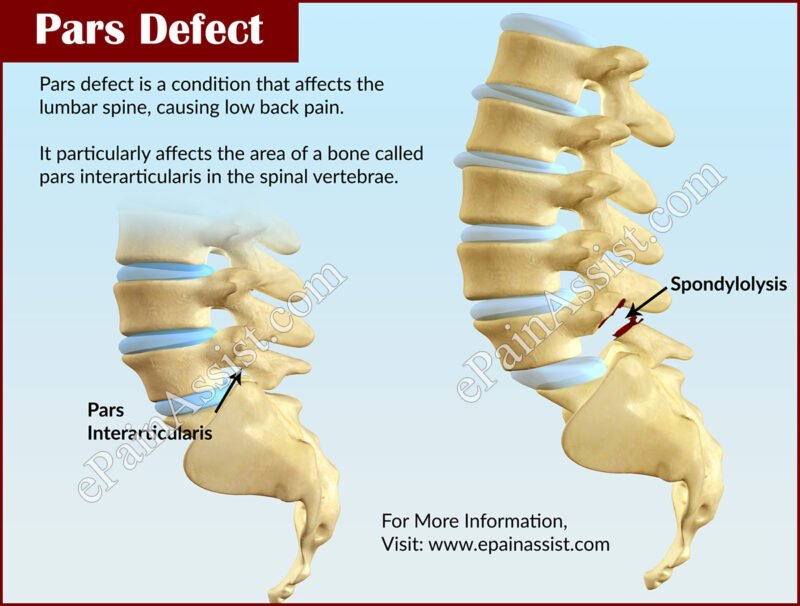
Patients also can present with neurogenic claudication symptomatology such as back and leg pain and discomfort associated with walking. However, the most common symptom of presentation is low back pain, which may be mechanical in nature. Many cases of isthmic spondylolisthesis are asymptomatic. Even more rare would be symptoms caused by central stenosis, given that most of these spondylolistheses rarely progress beyond grade II, and as the vertebral body translates anteriorly, the posterior elements tend to remain with the caudal vertebra maintaining their normal anatomic alignment. Other causes of symptoms can include lateral recess stenosis which, for example, can be caused by facet arthrosis or hypertrophied ligamentum flavum. Since the level most commonly affected is L5-S1, the L5 exiting nerve root in the L5-S1 foramen can be compressed. The radicular symptoms of isthmic spondylolisthesis are typically caused by the foraminal stenosis. These changes can result in back pain, neurogenic claudication and radiculopathy. This increased stress can lead to hypertrophy of the facet and ligamentum flavum. Spondylolisthesis can result in accelerated degeneration of the intervertebral disc which can lead to diminished height of the neural foramen and increased stresses on the facet joints posteriorly. Thus, risks associated with pars defects include activities associated with repetitive flexion/extension, axial loading, and rotational loading (i.e., golfers, weight lifers, baseball and football players, gymnasts). Pars fractures are believed to be the result of repetitive motion. These injuries can induce non-healing fractures or an elongated pars without a defect which likely indicates repeated fracture healing. Many biomechanical studies indicate that the pars is subjected to the greatest force of any structure in the lumbar spine therefore, it is susceptible to stress fractures which may heal and fracture repeatedly over time. This disconnection allows the anterior subluxation seen in spondylolisthesis. Thus, a defect in this structure would effectively “disconnect” the vertebral body above from the vertebral body below. Importantly, the facet joints of the superior and inferior vertebrae also are connected by the pars. The pars interarticularis, or pars, is the bony structure which connects the lamina, pedicle, and transverse processes of the vertebral bodies. The most common etiology for isthmic spondylolisthesis is instability of unilateral or bilateral pars interarticularis. The resulting anterior subluxation can produce back pain, central canal stenosis, and lateral recess or foraminal stenosis. Isthmic spondylolisthesis, which will be the topic of this discussion, refers to a defect in the pars interarticularis that then results in anterior subluxation over time, most commonly at L5-S1 followed by L4-5. There are many causes of spondylolisthesis including congenital, degenerative, traumatic, pathologic, iatrogenic, and isthmic. Grade 1 is less than 25%, Grade 2 is 25% to 50%, Grade 3 is 50% to 75%, Grade 4 is 75% to 100%, and Spondyloptosis is > 100%. Classification of Spondylolisthesis is based on the degree of slippage in the lumbar spine. The classification system utilized to categorize the degree of subluxation of the vertebral bodies is the Meyerding Classification, which quantifies the percentage of subluxation of the vertebral body above on the vertebral body below. When spondylolisthesis occurs acutely in the setting of traumatic or metastatic tumors, patients can present with neurological examination deficits including a loss of bowel and bladder function. The primary symptom of chronic spondylolisthesis is back pain, with or without leg pain. In most cases, symptoms associated with spondylolisthesis are chronic. Spondylolisthesis occurs when there is an anterior translation or “slippage” of one vertebral body relative to its caudal vertebral body. In other words, the anterior inferior endplate of the vertebral body above should be aligned with the anterior superior endplate of the vertebral body below. The lumbar spine in the sagittal plane should maintain an alignment in which each vertebral body is aligned with the vertebral body above and below. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
